From the article you will learn the features of varicose veins of the small pelvis in women - this is a deformation of the veins in the pelvic region with impaired blood circulation in the internal and external genitalia.
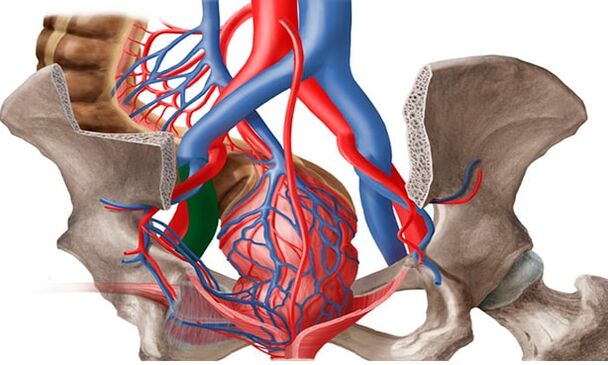
general informations
In the literature, varicose veins of the small pelvis are also called "pelvic congestion syndrome", "varicocele in women", "chronic pelvic pain syndrome". The prevalence of varicose veins of the small pelvis increases with age: from 19. 4% in girls under 17 to 80% in perimenopausal women. Most often, the pathology of the pelvic veins is diagnosed during the reproductive period in patients aged 25-45 years.
In the overwhelming majority of cases (80%), varicose transformation affects the ovarian veins and is extremely rare (1%) seen in the broad ligament veins of the uterus. According to modern medical approaches, the treatment of MTV should be carried out not so much from the point of view of gynecology, but first of all from the point of view of phlebology.
Pathology triggers
Under varicose veins of the pelvic organs in women, doctors understand a change in the structure of the vascular walls characteristic of other types of disease - weakening followed by stretching and the formation of "pockets" in which the blood stagnates. Cases where only the vessels of the pelvic organs are affected are extremely rare. In about 80% of patients, with this form, there are signs of varicose veins of the inguinal veins, vessels of the lower extremities.
The incidence of varicose veins of the small pelvis is more pronounced in women. This is due to anatomical and physiological features, suggesting a tendency for the weakening of the venous walls:
- hormonal fluctuations, including those associated with the menstrual cycle and pregnancy;
- increased pressure in the small pelvis, which is typical of pregnancy;
- periods of more active filling of the veins with blood, including cyclical menstrual periods, during pregnancy, as well as during sexual intercourse.
All these phenomena belong to the category of factors provoking varicose veins. And they are found exclusively in women. The greatest number of female patients face varicose veins of the small pelvis during pregnancy, since there is a simultaneous superposition of provoking factors. According to statistics, in men, varicose veins of the small pelvis are 7 times less common than in women. They have a more diverse set of provoking factors:
- hypodynamia - long-term preservation of low physical activity;
- increased physical activity, especially dragging weights;
- obesity;
- lack of sufficient fiber in the diet;
- inflammatory processes in the organs of the genitourinary system;
- sexual dysfunction or lucid refusal to have sex.
A genetic predisposition can also lead to the pathology of the plexuses located inside the small pelvis. According to statistics, varicose veins of the perineum and pelvic organs are most often diagnosed in women whose relatives suffer from this disease. The first changes can be seen in adolescence during puberty.
The greatest risk of developing inguinal varices in women with involvement of the pelvic vessels is observed in patients with venous pathology in other parts of the body. In this case, we are talking about congenital weakness of the veins.
Etiopathogenesis
Proctologists believe that the following main reasons still contribute to the onset of PVV: valve failure, venous obstruction, and hormonal changes.
Pelvic venous congestion syndrome can develop due to the absence or congenital insufficiency of venous valves, which has been revealed by anatomical studies in the last century, and modern data confirm this.
It was also found that in 50% of patients, varicose veins are genetic in nature. FOXC2 was one of the first genes identified that play a key role in the development of VVP. Currently, the relationship between disease development and gene mutations (TIE2, NOTCH3), thrombomodulin level and transforming growth factor β type 2 has been determined. These factors contribute to a change in the structure of the valve itself or the venous wall - all this leads to the failure of the structure of the valve; enlargement of the vein, which causes a change in valve function; with progressive reflux and finally with varicose veins.
An important role in the development of the disease can be played by connective tissue dysplasia, the morphological basis of which is a decrease in the content of various types of collagen or a violation of the ratio between them, which leads to a decrease in strengthvenous.
The incidence of PVV is directly proportional to the amount of hormonal changes, which are particularly pronounced during pregnancy. In pregnant women, the capacity of the pelvic veins increases by 60% due to the mechanical compression of the pelvic vessels by the pregnant uterus and the vasodilator effect of progesterone. This venous dilation persists for a month after childbirth and can cause venous valve failure. In addition, during pregnancy, the mass of the uterus increases, its position changes occur, which causes stretching of the ovarian veins, followed by venous congestion.
Risk factors also include endometriosis and other inflammatory diseases of the female reproductive system, estrogen therapy, unfavorable working conditions for pregnant women, which include heavy physical labor and prolonged forced posture (sittingor standing) during the working day.
The formation of varicose veins in the small pelvis is also facilitated by the anatomical features of the flow of the veins of the small pelvis. The diameter of the ovarian veins is usually 3 to 4 mm. The long, thin ovarian vein on the left flows into the left renal vein and on the right into the inferior vena cava. Normally, the left renal vein is located in front of the aorta and behind the superior mesenteric artery. The physiological angle between the aorta and the superior mesenteric artery is approximately 90 °.
This normal anatomical position prevents compression of the left renal vein. On average, the angle between the aorta and the superior mesenteric artery in adults is 51 ± 25 °, in children - 45, 8 ± 18, 2 ° in boys and 45, 3 ± 21, 6 ° in girls. If the angle decreases from 39. 3 ± 4. 3 ° to 14. 5 °, aorto-mesenteric compression, or nutcracker syndrome, occurs. This is called the anterior, or true, nutcracker syndrome that has the greatest clinical significance. Posterior nutcracker syndrome occurs on rare occasions in patients with retro-aortic or annular arrangement of the distal left renal vein. Obstruction of the proximal venous bed causes an increase in pressure in the renal vein, which leads to the formation of reno-ovarian reflux in the left ovarian vein with the development of chronic pelvic venous insufficiency.
May-Turner syndrome - compression of the left common iliac vein by the right common iliac artery - is also one of the causative factors of varicose veins in the pelvis. It occurs in no more than 3% of cases, it is more often found in women. Currently, due to the introduction of radiological and endovascular imaging methods in practice, this pathology is increasingly detected.
Classification
Varicose veins are subdivided into the following forms:
- The main type of varicose veins: an increase in blood vessels in the pelvis. The reason is valvular insufficiency of 2 types: acquired or congenital.
- The secondary form of thickening of the pelvic veins is diagnosed exclusively in the presence of pathologies in terms of gynecology (endometriosis, neoplasms, polycystic).
Varicose veins in the pelvis develop gradually. In medical practice, there are several main stages in the development of the disease. They will be different depending on the presence of complications and the spread of the disease:
- First degree. Changes in the structure of the valves of the ovarian vein may occur for hereditary reasons or may be acquired. The disease is characterized by an increase in the diameter of the veins up to 5 mm. The left ovary has a pronounced expansion in the outer parts.
- Second degree. This degree is characterized by the spread of pathology and damage to the left ovary. The veins in the uterus and the right ovary may also be dilated. The expansion diameter reaches 10 mm.
- Third degree. The diameter of the veins increases to 1 cm. Expansion of the veins is also observed on the right and left ovaries. This stage is due to pathological phenomena of a gynecological nature.
It is also possible to classify the disease according to the main cause of its development. There is a primary degree, in which the expansion is caused by faulty functioning of venous valves, and a secondary degree, which is the consequence of chronic female diseases, inflammatory processes or complications of an oncological nature. The degree of the disease may differ depending on the anatomical feature, which indicates the localization of the vascular disorder:
- Intra-caste plethora.
- Vulva and perineum.
- Combined shapes.
Symptoms and clinical manifestations
In women, pelvic varicose veins are accompanied by severe but nonspecific symptoms. Often the manifestations of this disease are considered signs of gynecological disorders. The main clinical symptoms of varicose veins in the groin in women with pelvic vessel involvement are:

- Non-menstrual pain in the lower abdomen. Their intensity depends on the stage of the venous lesion and the extent of the process. For the 1st degree of varicose veins of the small pelvis, periodic and mild pain, extending to the lower back, is characteristic. In the later stages, it is felt in the abdomen, perineum and lower back, and is long and intense.
- Profuse mucous discharge. The so-called leucorrhea does not have an unpleasant smell, does not change color, which would indicate infection. The discharge volume increases in the second phase of the cycle.
- Increased symptoms of PMS and dysmenorrhea. Even before the onset of menstruation, the pain in women increases, until the onset of difficulty in walking. During menstrual bleeding, it can become unbearable and spread to the entire pelvic area, perineum, lower back, and even thighs.
- Another characteristic sign of varicose veins in the groin in women is discomfort during sexual intercourse. It is felt in the vulva and vagina and is characterized by a dull ache. It can be observed at the end of intercourse. In addition, the disease is accompanied by increased anxiety, irritability and mood swings.
- As with varicose veins of the small pelvis in men, in the female part of patients with such a diagnosis, interest in sex gradually disappears. The cause of the dysfunction is both constant discomfort and a decrease in the production of sex hormones. In some cases, infertility can occur.
Instrumental diagnosis
Diagnosis and treatment of varicose veins is carried out by a phlebologist, a vascular surgeon. Currently, the number of cases of detection of PVV has increased due to new technologies. Patients with CPD are examined in several stages.
- The first step is a routine examination by a gynecologist: taking an anamnesis, manual examination, ultrasound examination of the pelvic organs (to exclude other pathologies). Based on the results, an examination is further prescribed by a proctologist, urologist, neurologist and other related specialists.
- If the diagnosis is not clear, but there is a suspicion of VVPT, at the second stage, a pelvic vein ultrasound angiography (USAS) is performed. It is a highly informative, non-invasive diagnostic screening method that is used in all women with suspected PTV. If previously it was believed that it was enough to examine only the pelvic organs (examination of the veins was considered difficult to access and optional), then at the present stage ultrasound of the pelvic veins is a mandatory examination procedure. . With the help of this method, it is possible to establish the presence of varicose veins of the small pelvis by measuring the diameters, the speed of blood flow in the veins and determining beforehand what is the main pathogenic mechanism - the failure ofovarian veins or venous obstruction. In addition, this method is used for the dynamic evaluation of conservative and surgical treatment of VVPT.
- The research is carried out by the transvaginal and transabdominal route. The parameter's veins, inguinal plexuses and uterine veins are visualized transvaginally. According to different authors, the diameter of the vessels of the named localizations varies from 2. 0 to 5. 0 mm (on average 3. 9 ± 0. 5 mm), that is. no more than 5 mm, and the average diameter of the arcuate veins is 1. 1 ± 0. 4 mm. Veins larger than 5mm in diameter are considered dilated. The inferior vena cava, iliac veins, left renal vein and ovarian veins are examined transabdominally to exclude thrombotic masses and extravasal compression. The length of the left renal vein is 6-10 mm, and its average width is 4-5 mm. Normally, the left renal vein where it passes over the aorta is somewhat flattened, but a decrease in its transverse diameter of 2 to 2. 5 times occurs without significant acceleration of blood flow, which ensures a flownormal without increasing the pressure in the prenosis. zoned. In case of stenosis of a vein against the background of pathological compression, there is a significant decrease in its diameter - from 3, 5 to 4 times, and an acceleration of blood flow - by more than 100 cm / s. The sensitivity and specificity of this method are 78 and 100% respectively.
- The examination of the ovarian veins is included in the compulsory examination of the pelvic veins. They are located along the anterior abdominal wall, along the rectus abdominis muscle, slightly outside the iliac veins and arteries. A sign of ovarian venous insufficiency in the USAS is considered to have a diameter greater than 5 mm with the presence of retrograde blood flow. For a complete examination, prevention of relapses and correct treatment tactics, ultrasound of the veins of the lower extremities, perineum, vulva, inner thigh and gluteal region should be performed.
- The development of medical technology has led to the use of new diagnostic methods. At the third stage, after ultrasound verification of the diagnosis, radiation diagnostic methods are used to confirm it.
- Pelvic venography with bilateral selective radiopaque ovarycography is one of the radio-invasive diagnostic methods that is only performed in a hospital setting. This method has long been considered the diagnostic gold standard for assessing dilation and detecting valve failure in pelvic veins. The essence of the method is the introduction of a contrast agent under the control of an X-ray installation through a catheter installed in one of the main veins (jugular, brachial or femoral) to the iliac veins, renal and ovarian. Thus, it is possible to identify the anatomical variants of the structure of the ovarian veins, to determine the diameters of the gonadal and pelvic veins.
- The retrograde contrast of the gonadal veins at the height of the Valsalva test serves as a pathognomonic angiographic sign of their valve insufficiency with visualization of strong expansion and tortuosity, respectively. This is the most accurate method for detecting May-Turner syndrome, post-thrombophlebitic changes in the iliac and inferior vena cava.
- When the left renal vein is compressed, the perirenal venous collaterals with retrograde blood flow in the gonadal veins, stagnation of contrast in the renal vein is determined. The method measures the pressure gradient between the left kidney and the inferior vena cava. Normally this is 1 mm Hg. From art. ; gradient equal to 2 mm Hg. Art. , may suggest slight compression; with a gradient >3 mm Hg. From art. can be diagnosed with aorto-mesenteric compression syndrome with hypertension in the left renal vein, and the gradient>5 mm Hg. From art. is considered a hemodynamically significant stenosis of the left renal vein. Determining the pressure gradient is an important part of the diagnosis, since, depending on its values, essentially different surgical interventions on the veins of the small pelvis are planned, which is very important in modern conditions. Currently, this study (with a normal pressure gradient) can be used for therapeutic purposes - for embolization of the ovarian vein.
- The next method of irradiation is emission computed tomography of the pelvic veins with labeled erythrocytes in vitro. It is characterized by the deposition of marked erythrocytes in the veins of the pelvis and visualization of the gonadal veins, allows to identify varicose plexuses of the small pelvis and dilated ovarian veins in various positions, the degree of pelvic venous congestion, refluxblood from the pelvic veins into the saphenous veins of the legs and perineum. Normally, the ovarian veins are not contrasted, the accumulation of the radiopharmaceutical in the venous plexuses is not observed. For an objective assessment of the degree of venous congestion of the small pelvis, the coefficient of pelvic venous congestion is calculated. But this method also has drawbacks: invasiveness, relatively low spatial resolution, impossibility of accurately determining the diameter of the veins, so it is not so often used in clinics at the present time.
- Laparoscopic video examination is a valuable tool for evaluating undiagnosed people. In combination with other methods, it can help determine the causes of pain and prescribe the appropriate treatment. With varicose veins of the small pelvis in the ovarian region, along the round and broad ligaments of the uterus, the veins can be visualized as cyanotic and dilated vessels with a thinned and strained wall. The use of this method is significantly limited by the following factors: the presence of retroperitoneal fatty tissue, the ability to assess varicose veins only in a limited area, and the inability to determine reflux from the veins. Currently, the use of this method is justified from a diagnostic point of view in case of suspicion of multifocal pain. Laparoscopy makes it possible to visualize the causes of CPD, for example, foci of endometriosis or adhesions, in 66% of cases.
Features of therapy
For the complete treatment of varicose veins of the small pelvis, a woman should follow all the doctor's recommendations and also make lifestyle changes. First of all, one should pay attention to the loads, if they are too high, they should be reduced, if the patient leads a too sedentary life, it is necessary to play sports, to walk more often, etc.
Patients with varicose veins are strongly advised to adapt their diet, to consume as little junk food as possible (fried, smoked, sweet in large quantities, salty. . . ), Alcohol, caffeine. It is better to give preference to vegetables and fruits, dairy products, cereals.
Also, as a prophylactic against the progression of the disease and for medicinal purposes, doctors prescribe the wearing of compression underwear for patients with varicose veins.
Medications
The therapy of ERCT involves several important points:
- get rid of the reverse flow of venous blood;
- relief of symptoms of the disease;
- stabilization of vascular tone;
- improvement of blood circulation in the tissues.
Preparations for varicose veins should be taken in progress. The rest of the drugs, which act as analgesics, are allowed to be drunk exclusively during a painful crisis. For effective treatment, the doctor often prescribes the following drugs:
- phleboprotectors;
- enzyme preparations;
- drugs that relieve inflammatory processes with varicose veins;
- pills to improve blood circulation.
Operative treatment
It should be recognized that conservative methods of treatment give really noticeable results, mainly in the early stages of varicose veins. At the same time, the problem can be fundamentally solved, and the disease can only be completely eliminated with surgery. In modern medicine, there are many variations of the surgical treatment of varicose veins, consider the most common and effective types of operations:
- embolization of the veins in the ovaries;
- sclerotherapy;
- plastic of uterine ligaments;
- removal of enlarged veins by laparoscopy;
- clamping of the veins of the small pelvis with special medical clips (clipping);
- crossectomy - venous ligation (prescribed if, in addition to the pelvic organs, the vessels of the lower extremities are affected).
During pregnancy, only symptomatic treatment of varicose veins of the small pelvis is possible. We recommend wearing compression tights, taking phlebotonics on the recommendation of a vascular surgeon. In trimester II-III, phlebosclerosis of varicose veins of the perineum can be performed. If, due to varicose veins, the risk of bleeding is high during spontaneous delivery, the choice is made in favor of operative delivery.
Physiotherapy
The system of physical activity for the treatment of varicose veins in a woman consists of exercises:
- "Bicycle". We lie on our backs, throw our hands behind our heads or place them alongside the body. Raising the legs, we perform circular movements with them, as if we were pedaling a bicycle.
- "Birch". We sit face up on any hard, comfortable surface. Lift your legs up and gently start them behind your head. Supporting the lumbar region with your hands and resting your elbows on the floor, slowly straighten your legs while lifting the body.
- "Scissors". The starting position is on the back. Lift the closed legs slightly above ground level. We spread the lower limbs to the sides, turn them over and repeat.
Possible complications
Why are varicose veins of the small pelvis dangerous? The following consequences of the disease are often recorded:
- inflammation of the uterus, its appendages;
- uterine bleeding;
- abnormalities in the work of the bladder;
- the formation of venous thrombosis (a small percentage).
Prophylaxis
In order for varicose veins of the small pelvis to disappear as quickly as possible, and in the future there will be no recurrence of the pathology of the pelvic organs, it is necessary to adhere to simple preventive rules:
- perform gymnastic exercises daily;
- prevent constipation;
- observe a diet in which plant fibers must be present;
- do not stay in one position for long;
- take a contrast shower of the perineum;
- so that varicose veins do not appear, it is better to wear exceptionally comfortable shoes and clothes.
Preventive measures aimed at reducing the risk of the appearance and progression of varicose veins in the small pelvis are mainly reduced to the normalization of lifestyle.




































